Pneumothorax
Pneumothorax is the presence of air in the pleural space, leading to lung collapse. It occurs when air leaks into the space between the visceral and parietal pleura, disrupting the negative pressure required for lung expansion.
Types of Pneumothorax:
Spontaneous Pneumothorax (Non-traumatic)
Primary: Occurs in individuals without underlying lung disease, often in tall, thin young males due to ruptured subpleural blebs.(small, air-filled blisters or cysts located on the outer layer of the lungs - the pleura)
Secondary: Occurs in patients with pre-existing lung disease (e.g., COPD, asthma, cystic fibrosis, tuberculosis).
Traumatic Pneumothorax
Blunt Trauma (e.g., rib fractures puncturing the lung).
Penetrating Trauma (e.g., stab or gunshot wounds).
Iatrogenic Causes (e.g., central line insertion, mechanical ventilation, lung biopsy, thoracentesis).
Tension Pneumothorax (Life-Threatening)
Progressive accumulation of air without escape, increasing intrapleural pressure, leading to mediastinal shift, reduced venous return, and cardiovascular collapse.
Requires emergency needle decompression followed by chest tube insertion.
Catamenial Pneumothorax
A rare form associated with menstruation, often linked to thoracic endometriosis - where endometrial tissue, typically found in the uterus, grows outside the pelvis, specifically in the chest cavity.
Clinical Presentation
Symptoms:
Sudden onset pleuritic chest pain
Dyspnea - shortness of breath (varies with severity)
Hypoxia (more common in secondary pneumothorax)
Signs:
Hyperresonance on percussion
Diminished breath sounds on the affected side
Decreased tactile fremitus (palpable vibration felt on the chest wall during speech or vocalization, assessed by placing hands on the patient's chest and having them speak).
Tracheal deviation (if tension pneumothorax)
Diagnosis:
Chest X-ray (CXR) – First-line Investigation
Visible pleural line with no lung markings beyond it.
Deep sulcus sign (in supine patients).
Mediastinal shift in tension pneumothorax.
Ultrasound (POCUS)
Absent lung sliding and barcode sign (M-mode).
CT Chest (if needed)
More sensitive, useful in small or complex cases.
Management:
Observation (Small, Stable Pneumothorax)
If less than 2 cm rim and patient is asymptomatic → Oxygen and monitoring.
Spontaneous resolution expected within days.
Needle Aspiration (Moderate Cases)
Indicated for primary pneumothorax if symptomatic.
Large-bore needle (14-18G) in 2nd ICS MCL (midclavicular line).
Chest Tube (Thoracostomy) – Definitive for Large or Unstable Cases
5th ICS, anterior axillary line (safe triangle).
Water-seal drainage prevents air re-entry.
Tension Pneumothorax – Emergency Management
Immediate needle decompression in 2nd ICS MCL → Followed by chest tube placement.
Surgical Management (for recurrent cases)
Pleurodesis (chemical or surgical)
Thoracotomy or VATS (Video-Assisted Thoracoscopic Surgery) for persistent leaks.
Spontaneous pneumothorax is a condition where the lung collapses due to accumulation of air or gas in the chest. The lung caves in due to inability to fill up with air during inhalation. This can happen to thin tall men without any prior symptoms. Spontaneous pneumothorax is more pronounced among men, especially smokers. Primary spontaneous pneumothorax occurs without any history of lung disease. It is usually attributed to the rupture of a air-filled sac within the lung. Secondary spontaneous pneumothorax is noticed among persons who are suffering from chronic obstructive pulmonary disease, tuberculosis, pneumonia, asthma, cystic fibrosis or lung cancer.
Primary spontaneous pneumothorax usually occurs in persons less than 40 years. On the other hand, secondary spontaneous pneumothorax is noticed among older patients. Sudden shock or low blood pressure or distended neck veins can bring on a condition of tension pneumothorax. This type of pneumothorax can also result from a serious accident or violent crime.
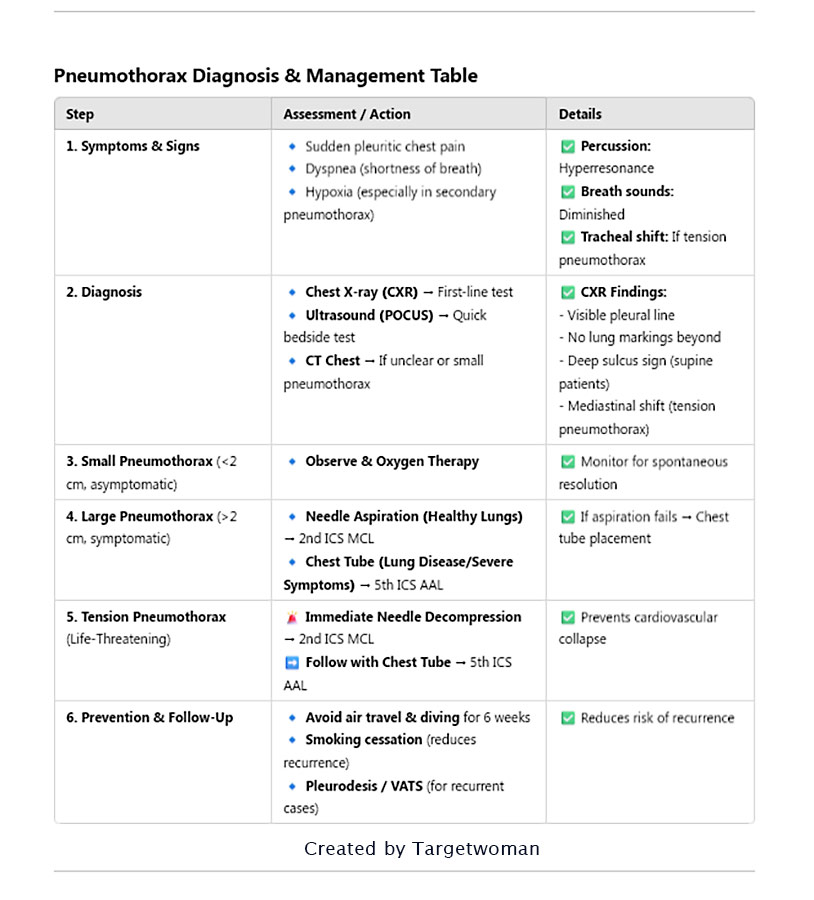
Breathlessness is the most prominent symptom of pneumothorax. There is dull or stabbing pain in the chest that is accentuated by coughing. A patient suffering from spontaneous pneumothorax experiences shortness of breath and abnormal breathing pattern. The patient feels agitated and enlarged neck veins will be observed. A physician will conduct a thorough physical examination and listen to your heart and breath sounds if he suspects a spontaneous pneumothorax condition. A chest x ray can confirm the collapse of the lung. The level of oxygen in the blood is measured with a pulse oximeter or an arterial blood gas analysis.
Treatment for spontaneous pneumothorax involves removal of air from the pleural space so as to allow the lungs to expand again. It may take several days for the lungs to re expand. A Catheter is used for aspiration of air from the pleural cavity. A chest tube is placed between the ribs to allow the air to be evacuated from that space. Doxycyline may be passed through the chest tube to seal the space.
- Quit smoking
- Avoid scuba diving and flying in aircrafts without sufficient pressure control
- Sleep with your head at elevated position
Thoracostomy
Thoracostomy is a procedure to decompress the pneumothorax or to drain pleural effusion.. Chest Thoracostomy is a life-saving technique that is resorted to in trauma cases. The tube is inserted into the pleural cavity to drain fluid, pus, blood or air. It is conducted for patients suffering Emphysema (irreversible lung disease where breathing becomes increasingly difficult), Pneumothorax (accumulation of air in pleural space), Chylothorax (milky lymphatic fluid in pleural space), Hydrothorax (accumulation of water in pleural space) and Pleural effusion.
Non invasive ventilation is usually the first line of therapy to avoid the intubation procedure in less severe cases. A peak expiratory flow rate (PEFR) assessment often is an useful adjunct to the physical examination of the patient with COPD (Chronic Obstructive Pulmonary Disease - progressive air way obstruction arising out of inflammatory pulmonary conditions).
Intubation : A tube is inserted into the pleural space by a physician who is trained in the procedure. The location of the insertion depends on whether air or fluid has to be drained. The area is cleaned and numbed. The tube is inserted between the ribs and the patient usually lies on the side or half sits up with the arm raised. The insertion site and the patient position depend on whether air or fluid is being drained. The tube is connected to a cannister into which the fluid or air is drained through suction. Often the chest tube insertion is guided by ultrasound or X-ray. Some of the possible risks of the Thoracostomy include bruising and bleeding of the chest wall and bacterial infection. Pulmonary or diaphragmatic laceration might occur.
Dyspnea
Dyspnea is commonly known as breathing difficulty or shortness of breath. It is noticed as difficulty in breathing or labored breathing. Tachypnea refers to rapid breathing. Progressively it can lead to hyperventilation such as experienced during an anxiety attack. Studies indicate that the origin of dyspnea is initiated with inaccurate central nervous system to the lungs with respect to breathing.
The etiology of dyspnea is related to conditions such as Pulmonary Embolism (PE), asthma, COPD, pulmonary ischemia and pneumonia. The management of dyspnea is only effective when the underlying causes are treated. In case of trauma, pneumothorax is an acute trigger for initiating the onset of dyspnea and hence emergency care is given to prevent internal bleeding that is caused in the pneumothorax. This condition can also progress into tachypnea and varied lung and heart sounds which has to be managed with effective ER procedures.
Positional dyspnea: If a person suffers dyspnea when lying down, it might be suggestive of CHF or pericardial effusion.
Exertional dyspnea: This occurs when there is reduction in oxygen supply and is mostly noticed in patients suffering cardiac disease or anemia.
Transient dyspnea: This situation usually resolves without medical intervention and is triggered by reversible causes such as panic attacks.
Recurrent dyspnea: Here the patient suffers these episodes many times.
Conditions such as pulmonary embolism can also lead to dyspnea along with tachycardia and diminished breathing patterns. Dyspnea is an immediate progressive condition usually associated with previous history of trauma or illness such as Tuberculosis, bronchopneumonia, infectious mononucleosis and sepsis in certain scenarios. Since dyspnea is an associated condition and it is predominantly an upper airway obstruction, the treatment measures are often related to avoiding exposure to chemicals, pollen, toxic fumes and gases such as carbon monoxide. Diagnostic tools such as Pulse Oximetry, blood tests for anemia, ECG and metabolic study are used to aid the diagnosis and then initiate appropriate treatment.
Tags: #Pneumothorax #Thoracostomy #Dyspnea
At TargetWoman, every page you read is crafted by a team of highly qualified experts — not generated by artificial intelligence. We believe in thoughtful, human-written content backed by research, insight, and empathy. Our use of AI is limited to semantic understanding, helping us better connect ideas, organize knowledge, and enhance user experience — never to replace the human voice that defines our work. Our Natural Language Navigational engine knows that words form only the outer superficial layer. The real meaning of the words are deduced from the collection of words, their proximity to each other and the context.
Diseases, Symptoms, Tests and Treatment arranged in alphabetical order:

A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
Bibliography / Reference
Collection of Pages - Last revised Date: May 26, 2026



