Sickle Cell Anemia
Sickle cell anemia is a hereditary condition characterized by destruction of red blood cells in the body. It is noticed that sickle cell anemia affects people of African ancestry and those of Mediterranean and Middle Eastern descent. The soft round red blood cells develop an abnormal shape that resembles a sickle or crescent moon. Their shape stops them from flowing easily and they get clogged up inside smaller blood vessels. This stops the blood from flowing properly. Important organs like the brain, heart, or kidneys need constant blood flow to stay healthy. Although our body attacks and destroys these sickle cells, it can't make new blood cells fast enough to replace the older ones. This results in the decrease in number of red blood cells leading to anemia. Sickle cell anemia is generally caused by genetic defects or disease. A child with sickle cell anemia has inherited a defective hemoglobin gene.
Sickle shaped blood cells get stuck within the small blood vessels and obstruct blood flow to some parts of the body, thereby leading to pain. Symptoms of sickle cell anemia include fatigue, breathlessness, rapid heart rate, delayed growth and puberty, susceptibility to infections, excessive penis pain, chest pain and decreased fertility. Since the spleen is damaged by the sickle cells, the resistance to infections is reduced considerably. Hands and feet tend to swell (Hand-foot syndrome) and the body faces stunted growth. Retinal damage can occur due to the obstruction of blood flow to the eyes. In about 10% of the cases, a stroke can occur if the sickle cells block blood vessels in the brain. Acute chest syndrome is another complication of this form of anemia. In this condition, the patient suffers symptoms similar to pneumonia and will need to be treated in a hospital.
There is no cure for sickle cell anemia but treatment can be followed to prevent complications and improve the quality of life of the patient. The patient will need to be under the guidance and care of a hematologist or genetic counselor. Blood test for hemoglobin 5 gives an indication as to the presence of this disease. A microscopic analysis of a blood sample will exhibit the distinctly shaped sickle cells. Bone marrow transplant can offer potential cure for this form of anemia, provided the right donor is found. Red blood cells from a donor can be given intravenously to a patient. But it carries inherent risks. Penicillin is given to keep young affected kids from life-threatening infections. Painkillers like acetaminophen and ibuprofen can relieve the pain associated with sickle cell anemia. Children diagnosed with sickle cell anemia must be given regular childhood vaccinations as well as Hib (Hemophilus Influenzae B) vaccine and the pneumococcal vaccine.
RDW blood test
Red blood cell (RBC) indices are calculations derived from the complete blood count that helps in the process of diagnosis and classification of Anemia. A RBC indices blood test requires 3 to 5 ml of blood collected from a vein puncture.
RDW (Red cell Distribution Width) blood test that calculates any variation in size of RBC. Normally Red Blood Cells are of a standard size. Since RBCs tend to get smaller and rounder as they age, it is not possible for all cells to be exactly the same size. RDW test determines the changes in the volume of the cells in the red cell population. The variations pertaining to the size of the red blood cells is called Anisocytosis and the shape is called Poikilocytosis.
The incidence of these conditions and the detection of abnormal or varied red blood size are determined by diagnostic blood smear analysis and also through automated analyzers.
The following are the normal results for red blood cell indices ( a measurement of the variation in size of red blood cells):
- Mean Corpuscular Volume (measure of the average volume of a RBC) : MCV 82-98 femtoliters (fl)
- Mean Corpuscular Hemoglobin Concentration (measurement of the average concentration of hemoglobin in a RBC) : MCHC 33-37 g/dl
- Mean Corpuscular Hemoglobin (Measurement of the average weight of hemoglobin in a RBC): MCH 26-34 picograms (pg)
- RDW 11.5-14.5%
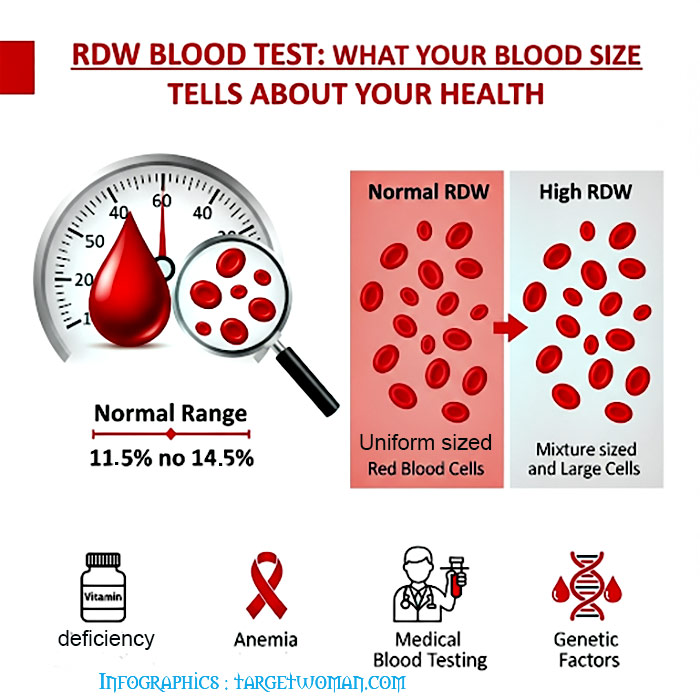
Normochromic: Indicates a normal concentration of hemoglobin. The RDW increases in anemia caused by deficiencies of Vitamin B12, iron or folic acid. Abnormal hemoglobin, as in sickle cell anemia, can result in changes in the shape of red blood cells. In addition it may also cause them to hemolyze. The abnormal shape and the cell fragments as a result of hemolysis would tend to increase the RDW. Severe blood loss may also induce immature cells into the blood that can increase the RDW.
Possible causes of abnormal MCV: MCV (Mean Corpuscular Volume) is an index of the size of the RBC. When the MCV is below normal, the RBC will be smaller than the normal size - which is known as microcytic. On the other hand, if the MCV is higher than normal, the RBC will also be larger than normal which is called as macrocytic while the normal RBC size is termed as normocytic.
High MCV: Macrocytic anemia owing to vitamin B12 and folic acid deficiency
Low MCV: Microcytic anemia, Thalassemia, poor iron content in diet and chronic illness
Normal MCV: Normocytic anemia owing to liver,kidney diseases, bone marrow disorders, hemolysis (distruction of red blood cells) or excessive bleeding
A low MCH (Mean Corpuscular Hemoglobin) is an indication that RBCs have too little hemoglobin. When viewed under the microscope, the RBCs appear pale and hence called as hypochromic. The MCHC (Mean Corpuscular Hemoglobin Concentration) is the ratio of RBC's hemoglobin mass to the cell volume. MCHC is elevated in hereditary Spherocytosis - as a result of the structural protein defect in the RBC.
Calculating Red Blood Cell Distribution: The determination of red cell distribution width is mathematically expressed as Red cell distribution width = (Standard deviation ÷ Mean cell volume) X 100.
Conditions such as pernicious anemia cause changes in RBC size. Often there is variation in shape too. This can be detected by changes in RDW. Normal RDW range is 11 - 15%. Higher RDW is indicative of disorders such as anemia. RDW blood test is often conducted along with MCV blood test to check the exact cause.
Phospholipids
Phospholipids are the principal components of cell membranes. These lipids form a bilayer enclosing the cytoplasm and other cell components and allow selective permeation into and out of the cell. These phospholipids protect the cell from chemicals, toxins, pathogens and free radicals. The phosphate head portion is hydrophilic (capable of mixing with water) while the lipid tail is hydrophobic; thus making phospholipids 'amphipathic'. Phospholipids are not triglycerides. Fatty acids are better absorbed from phospholipids as they dissolve in aqueous solutions. Phospholipids are often added to supplements and infant milk powder. Phospholipids are good carriers of Omega 3 PUFAs that are good for infant growth.
Tags: #Sickle Cell Anemia #RDW blood test #Phospholipids
At TargetWoman, every page you read is crafted by a team of highly qualified experts — not generated by artificial intelligence. We believe in thoughtful, human-written content backed by research, insight, and empathy. Our use of AI is limited to semantic understanding, helping us better connect ideas, organize knowledge, and enhance user experience — never to replace the human voice that defines our work. Our Natural Language Navigational engine knows that words form only the outer superficial layer. The real meaning of the words are deduced from the collection of words, their proximity to each other and the context.
Diseases, Symptoms, Tests and Treatment arranged in alphabetical order:

A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
Bibliography / Reference
Collection of Pages - Last revised Date: April 5, 2026



