Breast Cancer
Breast cancer is the second deadliest cancer among women. But it has been noted that with increased awareness and thereby early detection and improved treatment, the number of deaths has reduced. But the incidence of breast cancer has been increasing steadily. Breast cancer is generally noticed in women above the age of 50 years. If a woman has sisters, mother or close blood relatives who have had breast cancer, she is more at risk. Women who have had an early menarche and late menopause are at higher risk for breast cancer. Lifestyle factors such as high alcohol consumption, obesity, diet rich in saturated fat and sedentary lifestyle increases a woman's risk for breast cancer. Long-term use of Hormone Replacement Therapy or HRT increases the risk of breast cancer.
Approximately 8% of breast cancers are hereditary and of these one-half are associated with mutations in genes BRCA1 and BRCA2. A history of a proliferative breast abnormality like atypical Hyperplasia may increase the risk for developing breast cancer. Women who have a family history of BRCA mutation should initiate annual mammography between 25 and 35 years of age. The selective estrogen receptor modulator tamoxifen or raloxifene lowers the risk of developing breast cancer.
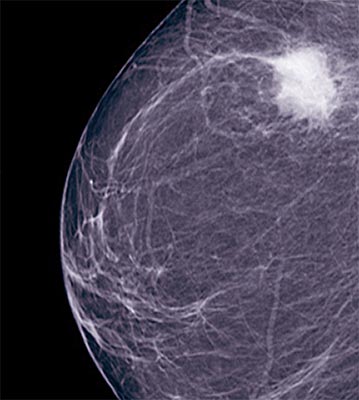
Symptoms of breast cancer:
- Lump or thickening in or near the breast or in the underarm area.
- Prominently visible veins on the surface of the breast or peeling and scaling should not be ignored.
- Yellowish green discharge from the nipple can be a possible breast cancer symptom.
- Nipple discharge may be from infection which is usually purulent and from pregnancy, stimulation or prolactinoma which produces a thin, milky, often bilateral discharge. A suspicious discharge from a single duct can be evaluated
with a ductogram.
- Change in size, shape and appearance need to be carefully observed, as it can be a potential symptom of breast cancer.
Every woman must learn to conduct a BSE (Breast Self Examination) to check for abnormal lumps, irregularities or discharge from the nipples. Such BSE combined with annual check ups by a doctor improves the chances of detecting breast cancer at an early stage. Palpate the breast tissue, axillary area and supra clavicular areas for masses or adenopathy. Physical examination of the breast should be performed in the upright and supine positions. Look for differences in size, retraction of the skin or nipple, prominent venous patterns and signs of inflammation. A mass that is suspicious for breast cancer is usually discrete, solitary, hard, unilateral and non tender. A Mammogram of the breast is routinely advised for women who are at higher risk for developing breast cancer. A clinically suspicious mass should be subjected to a biopsy even if mammography findings are normal.
Breast Cancer - Risk factors
- Family history of breast or ovarian cancer specifically with BRCA mutations
- History of breast cancer
- Increasing age
- Early age at menarche and late menopause.
- Prolonged exposure / higher concentrations of endogenous or exogenous estrogen
- Exposure to ionizing radiation
- Dense breast tissue
- atypical Hyperplasia
- Women with no children or who had their first child after the age 30
- Sedentary life style
- High fat content in diet
- Excessive Alcohol consumption
Though Bilateral mastalgia is rarely associated with breast cancer, it does not totally rule out the possibility. It is usually related to Fibrocystic changes in pre menopausal women with diffuse lumpy breasts.
Breast Cancer - Treatment Options
Appropriate breast cancer treatment is decided on the basis of a number of factors. Breast cancer treatment will depend on a number of factors such as size and location of the breast lump, the stage at which it was detected and the results of hormone receptor tests.
The most common approach for advanced breast cancer is preoperative chemotherapy followed by surgery and radiotherapy.
Surgery and chemotherapy are often used in combination. Chemotherapy is breast cancer treatment with anti-cancer drugs administered intravenously or orally. This systemic form of treatment is either administered alone or along with surgical procedures. Chemotherapy is a systemic therapy that affects the entire body by entering the bloodstream. This is used widely in breast cancer treatment to interfere with rapidly dividing cells. Radiation is the use of high-energy rays to prevent breast cancer cells from further growth and division. Though normal cells are also affected by this form of breast cancer treatment, they generally repair themselves and function normally afterwards. Adjuvant systemic therapy consists of administration of hormone
therapy, chemotherapy or trastuzumab (a monoclonal antibody directed against HER-2/neu). It benefits most women who are in the early stage of breast cancer, but the magnitude of benefit is greatest for those with node positive disease.
Salivary Gland Cancer
There are hundreds of minor salivary glands lining parts of the mouth and larynx and can be seen only though a microscope. Many of the salivary gland tumors are non cancerous and they do not spread to other tissues. Salivary gland cancer is a type of head and neck cancer. Advancing age, radiation therapy to head and neck and exposure to cancer-causing chemicals at work are largely factors that cause salivary gland cancer.
Causes and risk factors
Risk of getting salivary gland cancer increases as one gets older. Most develop it in their 50s and 60s. A person is at higher risk of developing salivary gland cancer if exposed to radiation. One may also come in contact with radioactive substances through work. In case of childhood cancer and treatment with radiotherapy, there is increased risk for at least 20 years post treatment. Skin cancer in the past also slightly increases the risk of cancer of salivary glands. Smoking tobacco tends to increase the risk. Human papilloma virus has been noticed in some types of salivary cancer and efforts are on to confirm this. Investigation into the low level radiation from mobile phones is also being done.
Signs and symptoms
While salivary gland cancer may not cause any symptoms, it is sometimes found during a regular dental check up. As symptoms caused by salivary gland cancer may also be caused by other conditions, consult a doctor if any of the following problems occur:
- A painless lump in the area of the ear, cheek, jaw, lip or inside the mouth
- Fluid draining from the ear
- Numbness in the face
- Weakness in the face
- Persistent pain in the face
- Trouble swallowing or opening the mouth wide.
Diagnosis
CT and MRI are used to determine if salivary gland cancer has spread to other tissues. An examination of the patient to check signs of health, in the neck, mouth and throat areas is vital. History of patient's health, habits and past illnesses and treatments is recorded. A small amount of glucose is injected into the vein and the PET (Positron Emission Tomography) scanner rotates around the body and takes images where glucose is used in the body. Malignant cells show up brighter in the picture because they are more active and take up more glucose than normal cells do. Endoscopy and biopsy are also done to test for salivary gland cancer. As salivary gland cancer is hard to diagnose, it is recommended to have tissue samples checked by a pathologist who has expertise in diagnosing salivary gland cancer.
Treating salivary gland cancer
Stage I is when cancer is confined to the salivary glands and is 2 cm or smaller; Stage II is larger than 2 cm but not larger than 4 cm; stage III is when it has spread to a lymph node or to soft tissues around the affected gland and stage IV has spread further.
There are three types of standard treatment used for salivary gland cancer – surgery, radiation therapy and chemotherapy. Some may receive more than one type of treatment. Therapy depends upon the stage the patient is in and the higher the stage, more the therapy and aggressive and multiple therapies are given.
Surgery
If the tumor is small and located in an easy-to-access spot, surgeon may remove it and a small portion of healthy tissue that surrounds it. Removing the entire salivary gland is done if the tumor is large and if the cancer extends to nearby structures such as facial nerves, ducts that connect to salivary glands, facial bones and skin may also be removed.
If the cancer has spread to lymph nodes in the neck, the surgeon may remove most of the lymph nodes. Reconstructive surgery is done by a plastic surgeon to improve the ability to chew, swallow, speak and breathe after the surgery. The patient may need grafts of skin, tissue or nerves from other parts of the body to rebuild areas in the mouth, throat and jaw.
Radiation therapy
Radiation therapy using neutrons which are more effective in treating certain salivary gland cancers is used. Post surgery, this therapy is used to kill cancer cells that might still remain. In case surgery is not possible and tumor is large and located in a place that makes removal too risky, radiation alone is used to treat salivary gland cancer.
Chemotherapy
Although this is not currently used as a standard treatment for salivary gland cancer, Chemotherapy is a drug treatment used to kill cancer cells. This may be an option for people with advanced salivary gland cancer that has spread to distant areas in the body.
Those who undergo radiation therapy to the head and neck often experience dry mouth which can be uncomfortable. This can lead to frequent infections in the mouth, cavities and pose problems in teeth and difficulty eating, swallowing and speaking. If such complications arise then:
- Brush teeth several times a day.
- Rinse mouth with warm salt water after each meal.
- Keep mouth moistened with water or sugarless candies.
- Choose moist food and moisten dry food with sauce, gravy, broth, butter or milk.
- Avoid acidic or spicy foods and drinks, such as caffeinated and alcoholic beverages.
Brain Cancer
Malignant tumors in the brain are the consequence of abnormal growth of cells in the brain. Brain cancers can be primary, arising from primary brain cells, or from other brain components. Metastatic brain cancer starts elsewhere in the body and spreads to the brain. About 25% of tumors elsewhere in the body metastasize to the brain. The most common cancers that metastize to the brain are lung cancer, breast cancer, colon cancer and melanoma. The majority of brain metastases are located in the cerebral hemispheres and then in the cerebellum. Very few occur in the brain stem.
Causes/ risk factors for brain cancer
- Any radiation to the head
- Hereditary
- HIV infection
- Smoking
- Toxins found in the environment such as chemicals in oil refinery, rubber industry chemicals etc)
Symptoms of Brain Cancer
- Severe headache in the morning.
- Nausea and vomiting, especially early in the mornings.
- Some changes/problems while talking, listening or seeing.
- Problems while walking.
- Memory problems or lack of alertness.
- Twitching of muscles or seizures.
- Numbness in the arms or legs.
- General weakness
- Clumsiness
- Gradual changes in intellectual and emotional capacity.
These symptoms may be very gradual and therefore overlooked by the patient. Occasionally however, these symptoms may appear more rapidly.
Who is at risk for brain cancer ?
Persons with the following conditions are at more risk for developing cancer of the brain.
- Frequent exposure to radiation
- Age
- Exposure to pesticides, herbicides and fertilizer
- Workers occupied in petroleum, plastic, rubber and textile industries.
- Exposure to electromagnetic fields
- Genetic disorders
Diagnosis of Brain Cancer
MRI has higher sensitivity for detecting the presence and characteristics of a tumor. In case, the CT or MRI indicates the presence of a brain tumor, the patient will be referred to a neurosurgeon or to a neuro oncologist. The next step in diagnosis is to confirm cancer in the brain. A biopsy is taken to identify the type of tumor and the grade of the tumor. This is done by a surgical procedure called craniotomy. The skull is opened with the intention of removing the whole tumor if possible. A biopsy is taken from the tumor. In some cases, if the exact location of the tumor is detected, by using a CT or MRI scan, a biopsy is taken without opening the skull. This technique is stereotaxis, where a needle is used to collect the biopsy. A pathologist examines the biopsy under a microscope and diagnoses the disease.
Brain cancer treatment
Treatment for brain cancer is based on the patient's age, and general health status, size, location and type and grade of the tumor. In most cases of brain cancer, surgery, radiation and chemotherapy are the preferred treatment. As treatment protocols of brain cancer are highly complex, most treatment plans will involve several consultations and sittings with the neurosurgeon, oncologist, radiation oncologist and healthcare provider.
Most people with brain cancer undergo surgery to assign and grade the tumor and then remove the tumor or take a sample to identify the type and grade. In some cases, a benign tumor can be cured by surgical intervention and removal of tumor.
Stereotactic radio surgery, a knife less technique that can destroy a brain tumor without opening the skull can be adopted. With a CT or MRI, the exact location is pinpointed and with high energy radiation beams the tumor from different angles is destroyed. Knife less procedure has fewer complications and the recovery time is shorter. The disadvantage is the lack of tissue available to send to a pathologist for diagnosis of brain swelling.
Radiation can be administered externally or internally. External radiation travels through skin and the skull, healthy brain tissue and other tissues to get to the tumor. Internal radiation uses a tiny radioactive capsule placed inside the tumor itself. The radiation emitted from the capsule destroys the tumor.
Chemotherapy drugs may be administered by mouth or through an IV line. Chemotherapy is usually administered in cycles, each cycle consisting of a short period of intensive treatment followed by a period of rest and recovery. The side effects of chemotherapy include nausea, vomiting, mouth sores, loss of appetite, loss of hair among others. New therapies with the use of nanotechnology for cancer are being developed and are promising. Regular follow up is essential after treatment of brain cancer. Such checkups would include physical and neurologic exams, and occasional CT and/or MRI.
Tags: #Breast Cancer #Salivary Gland Cancer #Brain Cancer
At TargetWoman, every page you read is crafted by a team of highly qualified experts — not generated by artificial intelligence. We believe in thoughtful, human-written content backed by research, insight, and empathy. Our use of AI is limited to semantic understanding, helping us better connect ideas, organize knowledge, and enhance user experience — never to replace the human voice that defines our work. Our Natural Language Navigational engine knows that words form only the outer superficial layer. The real meaning of the words are deduced from the collection of words, their proximity to each other and the context.
Diseases, Symptoms, Tests and Treatment arranged in alphabetical order:

A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
Bibliography / Reference
Collection of Pages - Last revised Date: June 9, 2026



