Breast Cancer
Breast cancer is the second deadliest cancer among women. But it has been noted that with increased awareness and thereby early detection and improved treatment, the number of deaths has reduced. But the incidence of breast cancer has been increasing steadily. Breast cancer is generally noticed in women above the age of 50 years. If a woman has sisters, mother or close blood relatives who have had breast cancer, she is more at risk. Women who have had an early menarche and late menopause are at higher risk for breast cancer. Lifestyle factors such as high alcohol consumption, obesity, diet rich in saturated fat and sedentary lifestyle increases a woman's risk for breast cancer. Long-term use of Hormone Replacement Therapy or HRT increases the risk of breast cancer.
Approximately 8% of breast cancers are hereditary and of these one-half are associated with mutations in genes BRCA1 and BRCA2. A history of a proliferative breast abnormality like atypical Hyperplasia may increase the risk for developing breast cancer. Women who have a family history of BRCA mutation should initiate annual mammography between 25 and 35 years of age. The selective estrogen receptor modulator tamoxifen or raloxifene lowers the risk of developing breast cancer.
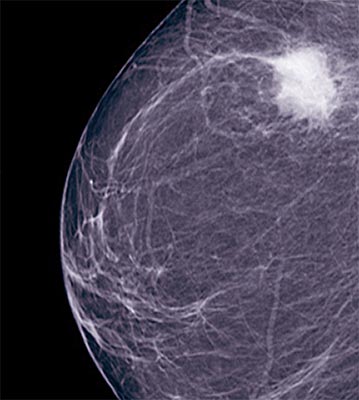
Symptoms of breast cancer:
- Lump or thickening in or near the breast or in the underarm area.
- Prominently visible veins on the surface of the breast or peeling and scaling should not be ignored.
- Yellowish green discharge from the nipple can be a possible breast cancer symptom.
- Nipple discharge may be from infection which is usually purulent and from pregnancy, stimulation or prolactinoma which produces a thin, milky, often bilateral discharge. A suspicious discharge from a single duct can be evaluated
with a ductogram.
- Change in size, shape and appearance need to be carefully observed, as it can be a potential symptom of breast cancer.
Every woman must learn to conduct a BSE (Breast Self Examination) to check for abnormal lumps, irregularities or discharge from the nipples. Such BSE combined with annual check ups by a doctor improves the chances of detecting breast cancer at an early stage. Palpate the breast tissue, axillary area and supra clavicular areas for masses or adenopathy. Physical examination of the breast should be performed in the upright and supine positions. Look for differences in size, retraction of the skin or nipple, prominent venous patterns and signs of inflammation. A mass that is suspicious for breast cancer is usually discrete, solitary, hard, unilateral and non tender. A Mammogram of the breast is routinely advised for women who are at higher risk for developing breast cancer. A clinically suspicious mass should be subjected to a biopsy even if mammography findings are normal.
Breast Cancer - Risk factors
- Family history of breast or ovarian cancer specifically with BRCA mutations
- History of breast cancer
- Increasing age
- Early age at menarche and late menopause.
- Prolonged exposure / higher concentrations of endogenous or exogenous estrogen
- Exposure to ionizing radiation
- Dense breast tissue
- atypical Hyperplasia
- Women with no children or who had their first child after the age 30
- Sedentary life style
- High fat content in diet
- Excessive Alcohol consumption
Though Bilateral mastalgia is rarely associated with breast cancer, it does not totally rule out the possibility. It is usually related to Fibrocystic changes in pre menopausal women with diffuse lumpy breasts.
Breast Cancer - Treatment Options
Appropriate breast cancer treatment is decided on the basis of a number of factors. Breast cancer treatment will depend on a number of factors such as size and location of the breast lump, the stage at which it was detected and the results of hormone receptor tests.
The most common approach for advanced breast cancer is preoperative chemotherapy followed by surgery and radiotherapy.
Surgery and chemotherapy are often used in combination. Chemotherapy is breast cancer treatment with anti-cancer drugs administered intravenously or orally. This systemic form of treatment is either administered alone or along with surgical procedures. Chemotherapy is a systemic therapy that affects the entire body by entering the bloodstream. This is used widely in breast cancer treatment to interfere with rapidly dividing cells. Radiation is the use of high-energy rays to prevent breast cancer cells from further growth and division. Though normal cells are also affected by this form of breast cancer treatment, they generally repair themselves and function normally afterwards. Adjuvant systemic therapy consists of administration of hormone
therapy, chemotherapy or trastuzumab (a monoclonal antibody directed against HER-2/neu). It benefits most women who are in the early stage of breast cancer, but the magnitude of benefit is greatest for those with node positive disease.
Mastectomy
Mastectomy is a surgical procedure to treat breast cancer. The appropriate mastectomy procedure is decided after considering the woman's age and general health along with the tumor size, stage and grade. In early stages of breast cancer, partial mastectomy is performed and followed with radiation therapy on remaining breast tissues. Lumpectomy involves removal of only the tumor along with a small portion of surrounding tissue. This tissue along with nearby lymph nodes are examined for guiding future treatment course. While unilateral mastectomy involves surgical removal of one breast, bilateral mastectomy means removal of both breasts. When this is done, the breast tissue is also removed so as to reduce the chances of breast cancer from recurring.
Prophylactic mastectomy means removing healthy breasts of a woman so as to reduce the chances of developing breast cancer. This is done in high-risk women after consultation with a specialist in cancer genetics. Women who have already had breast cancer or have a family history of breast cancer may consider this procedure to reduce their risks. This procedure is also referred to as preventive mastectomy. With existing data it is noticed that prophylactic mastectomy reduces the risk of breast cancer by 90% in moderate and high-risk women.
Oncotype DX
Oncotype DX test measures the levels of specific genes that may indicate the presence of cancer cells. This test helps check the risk of recurrence of breast cancer. This test makes use of breast cancer biopsy and studies the patient where the cancer is hormone-receptor positive. Then the Oncotype DX test draws up a recurrence score. A high recurrence score indicates higher chances of cancer recurrence. But this has to be seen along with other factors such as the age of the patient, grade of cancer and size of cancer. This test costs about $3,500. In many cases, the Oncotype DX test helps in deciding whether a woman must go in for chemotherapy and hormonal therapy post surgery for breast cancer. Typically those with low recurrence score may not need to undergo chemotherapy. The Oncotype DX test aids in tailoring treatment to suit the individual needs of each patient.
Tags: #Breast Cancer #Mastectomy #Oncotype DXAt TargetWoman, every page you read is crafted by a team of highly qualified experts — not generated by artificial intelligence. We believe in thoughtful, human-written content backed by research, insight, and empathy. Our use of AI is limited to semantic understanding, helping us better connect ideas, organize knowledge, and enhance user experience — never to replace the human voice that defines our work. Our Natural Language Navigational engine knows that words form only the outer superficial layer. The real meaning of the words are deduced from the collection of words, their proximity to each other and the context.
Diseases, Symptoms, Tests and Treatment arranged in alphabetical order:

A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
Bibliography / Reference
Collection of Pages - Last revised Date: July 5, 2025



