Pacemaker
The heart works on the natural electrical impulses by the cardiac conduction system. An electronic pacemaker is surgically implanted in some patients suffering from cardiac arrhythmia to regulate the heart rhythm. This is done with electrical impulses generated by the pacemaker. The pacemaker system is made up of a battery pack and a couple of thin wires. The small generator is implanted under the skin. This is connected to the heart through tiny wires. The pacemaker ensures regular impulses to the heart so that they appear just like the natural pacemaker of the heart.
Demand pacemakers are those that are used only when needed. They have sensors that that kick off their pacemaker when the heart rhythm is slower than the required rate. Rate-responsive cardiac pacemakers automatically regulate the heart beat according to the body's need. It is imperative to check the functioning of the pacemaker regularly. The doctor will also need to detect any signs of the batteries wearing off. Certain medications, electrical device or electromagnetic noise can interfere with the working of the cardiac pacemaker. Handheld metal detectors, cellular phones and MRI can affect the pacemaker.
Deep Brain Stimulation
Deep brain stimulation is a specialized neurosurgical treatment option for patients suffering from a special group of neurological disorders called 'Movement Disorders'. Deep Brain Stimulation or DBS is an advanced procedure performed by neurosurgeons for treating patients who cannot achieve optimal results through conventional medical therapy alone.
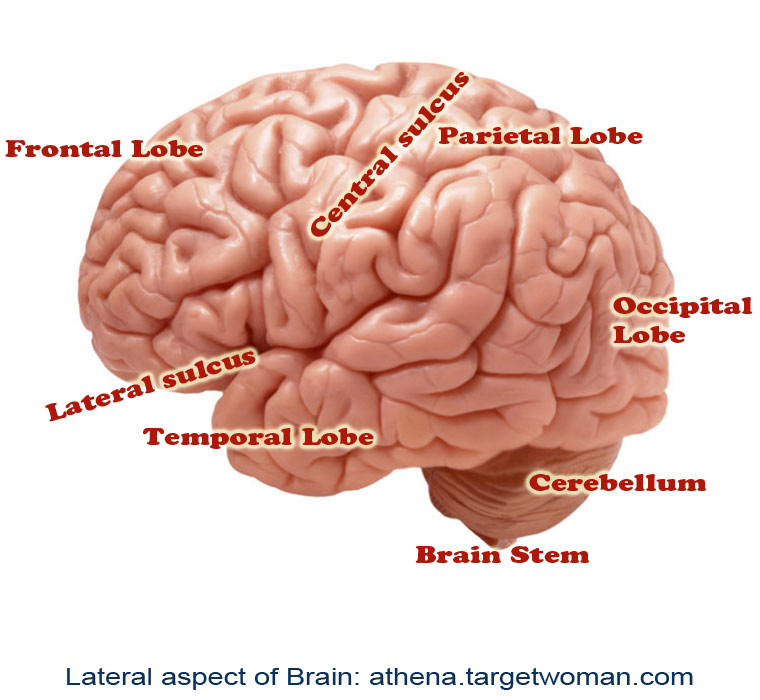
Neurophysiology of Movement Disorders
Movement disorders refer to conditions associated with changes in specific areas of the nervous system which results in abnormal involuntary movements, slow or reduced movements. The two main areas of the brain which are affected in movement disorders are the basal ganglia and the sub-thalamic nucleus. The disorders are classified into various groups such as hypokinetic disorders (e.g.: Parkinsons), hyperkinetic disorders (e.g.: Huntington's disease), and Non-motor disorders (e.g.: Tourette's Syndrome and Obsessive Compulsive Disorders). When these nuclei start having abnormal electrical activity (discharging too much or too little), the patient experiences specific symptoms related to movement.
Indications for Deep Brain Stimulation
Deep brain stimulation is used for patients who usually suffer from movement disorders such as Parkinsons, tremors, and dystonia. It is called Deep Brain Stimulation because surgically placed electrodes are used to stimulate specific areas (nuclei) deep inside the brain. The most common nuclei commonly stimulated are the Globus Pallidus and the sub-thalamic nuclei.
The idea behind DBS is that it functions somewhat like a 'pacemaker' in the brain, periodically sending electrical signals to the specific nuclei, thereby modulating the effect of these nuclei. Hence, DBS is also called as neuromodulation therapy'. In DBS, specific electrical signals are sent to the abnormally functioning nuclei to reduce or increase their activity.
Components
There are three components of the Deep Brain Stimulation system. They are:
The Stimulating Electrodes
The IPG – Internal Pulse Generator (the pacemaker)
The Extension - connecting leads between the Electrode and IPG.
The IPD contains a battery pack which has to be replaced every 4 years. The IPG is programmed by the neurologist based on the specific disease condition of the patient, and the placement of DBS requires regular follow-ups for programming the IPG based on the disease condition, if needed.
Procedure
Specialized Brain Mapping technology is used to locate the specific nuclei which are suspected to be abnormally functioning. These nuclei are the 'target area' for DBS. A specially designed stereotaxic frame is attached to the patient's head which provides a three-dimensional reference system for the patient's brain and enables the neurosurgeon to precisely locate the nuclei or track the electrode tip during placement.
The procedure normally takes up to three hours and is performed by a neurosurgeon specially trained in the procedure. The surgery is called awake craniotomy since the patient is awake during the entire duration of the procedure so that his neurological functions can be assessed in real-time to see the 'before and after' results due to the electrode placement. Following the placement of the electrodes, the IPGs are implanted either during the time of the surgery or later on. Each brain is unique, and hence the IPGs have to be specially programmed and the settings have to be specific for each patient. This is usually done about 2 weeks after the electrode placement.
Clinical Results
It is not exactly known how DBS functions, but there have been marked clinical improvements for patients with Parkinson's disease, tremors, and dystonia. Although a large percentage of patients report significant improvement after DBS surgery, there is no guarantee that DBS will help every patient with movement disorder.
Patients with Parkinson's report 60-80% improvement in tremor and slowness of movement. Patients on an average report 50% improvement in their walking and balance following DBS. Others with dyskinesia (involuntary movements) report more than 80% improvement following DBS.
Complications
Although DBS on the whole has proven safe and effective, there is a possible 2-3% risk of intra-cranial hemorrhage and meningitis due to leakage of cerebro-spinal fluid. There is a 15% chance of developing infection due to the placement of the electrodes. There is a possibility that seizures may occur, if the tip of the electrode migrates, thereby stimulating other areas of the brain. However such findings have not been reported until now.
Future of DBS
Besides movement disorders, DBS has been used to chronic pain, and currently possibilities of using DBS for other cognitive disorders such as severe depression, obsessive compulsive disorder, eating behavioral disorders and drug addiction, are underway.
Cardiac Arrhythmia
Cardiac arrhythmia or Cardiac dysrhythmia refers to a disturbance of the heart rhythm. When the regular heart rhythm is disturbed, it can lead to symptoms that can range from mild to life-threatening. The heart may have slower beats or there may be a blockage of the electrical pathway of the heart. One of the most common form of cardiac arrhythmia is atrial fibrillation. This occurs in older persons when the upper atrial chambers of the heart do not pump correctly. This can lead to blood clots. Heart failure or electrolyte imbalance can bring on cardiac arrhythmia.
Tachycardia or Tachydysrhythmia is a condition where there is rapid heartbeat due to inefficiency in the blood circulation. Tachycardia is a condition where the heart rhythm is more than 100 beats/minute. This can happen due to stress, hyperthyroidism or alcohol. On the other hand, Bradycardia or bradyarrhythmia is a condition where the heart rhythm is less than 60 beats/min. A ventricular arrhythmia can be life-threatening. This happens when there is ventricular fibrillation. It is essential to treat this condition and restore the rhythm within minutes to prevent heart damage and death. Allergic reactions can trigger arrhythmia.
Some persons suffering from cardiac arrhythmia notice symptoms such as dizziness, fainting and lightheadedness. There may be a fluttering or pounding sensation in the chest. Anti arrhythmic agents such as amiodarone and sotalol are prescribed to maintain the normal rhythm of the heart. Amiodarone is effective atrial flutter and to establish heart's normal rhythm.
In cases of atrial fibrillation, Warfarin is used to prevent blood clots. Medication for cardiac dysrhythmia includes beta blockers such as metoprolol and atenolol to reduce the heart rhythm. An electronic cardiac pacemaker may be implanted to regulate the heart beat.
Tags: #Pacemaker #Deep Brain Stimulation #Cardiac Arrhythmia
Enter your health or medical queries in our Artificial Intelligence powered Application here. Our Natural Language Navigational engine knows that words form only the outer superficial layer. The real meaning of the words are deduced from the collection of words, their proximity to each other and the context.
Diseases, Symptoms, Tests and Treatment arranged in alphabetical order:

A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
Bibliography / Reference
Collection of Pages - Last revised Date: April 25, 2024



